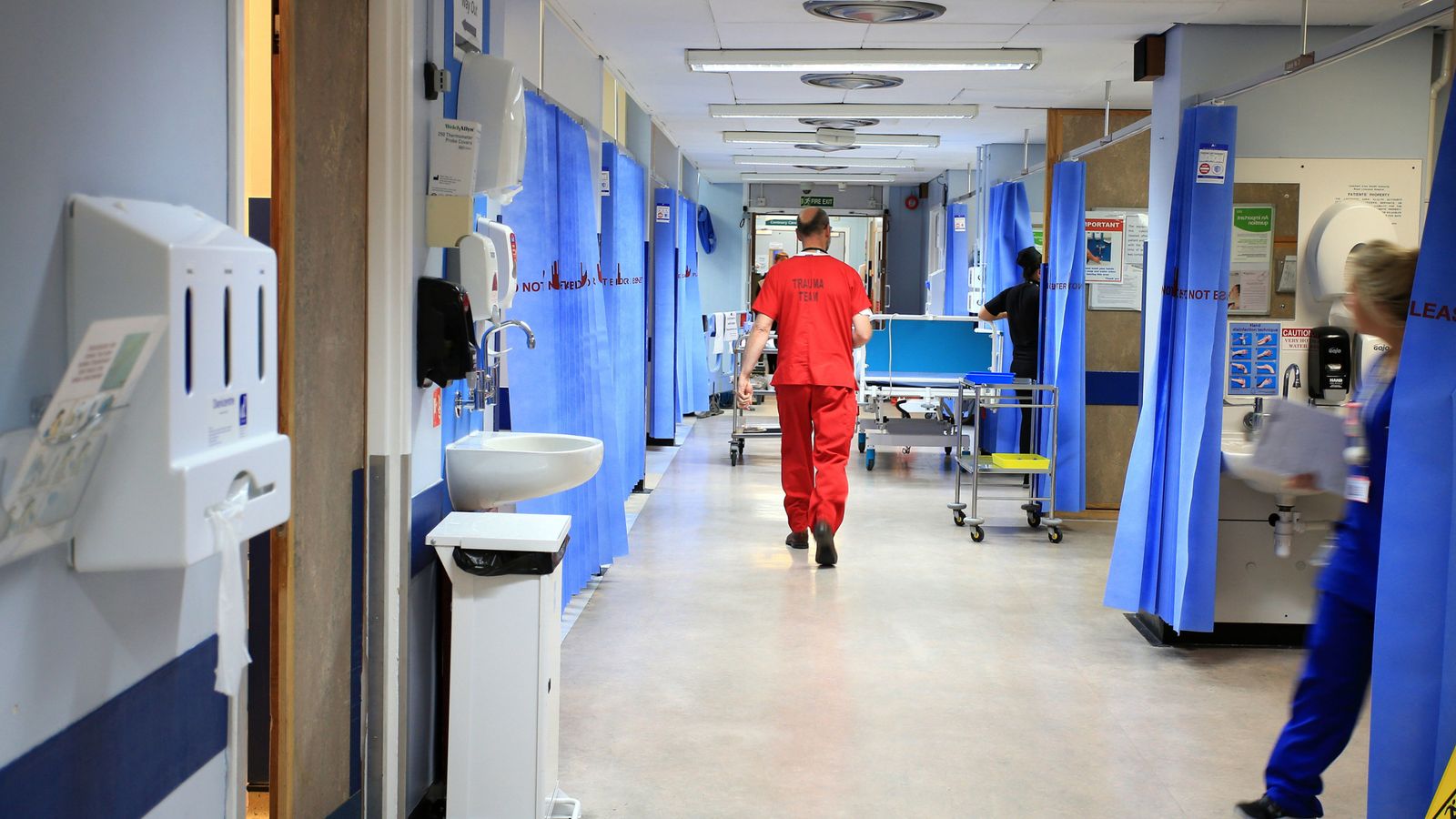
NHS waiting lists for elective care could more than double to reach 12 million by March 2025 due to the pandemic backlog, a National Audit Office (NAO) report has warned.
Despite the government providing an additional £8bn from 2022 to 2025 to support the recovery of elective care – procedures that are planned in advance – the independent spending watchdog said the best-case scenario will still see waiting lists of seven million by March 2025.
Since the pandemic, the NAO found NHS waiting lists for procedures like hip replacements or tonsil removal reached a record 5.83 million by September 2021 – up from 4.43m in February 2020 before the start of the pandemic.
Of those patients waiting, 1.95m were waiting for more than the 18-week maximum target and 301,000 were waiting for more than a year.
By June 2021, cancer services had recovered to pre-pandemic levels but patients with an urgent GP referral for cancer were more likely to be delayed, with 26% having to wait more than the 62-day target to start up to September 2021.
The NAO also predicted there were between 240,000 and 740,000 “missing” urgent GP referrals for suspected cancer during the pandemic as people avoided seeking, or were unable to obtain, referrals.
And it estimates up to September 2021, between 35,000 and 60,000 fewer people started cancer treated than would have been expected, while there were between 7.6m and 9.1m fewer elective care referrals.
COVID-19: Some Omicron cases have ‘mild’ symptoms and experts should know more about transmission in coming days – WHO
COVID-19: Travel stocks lead FTSE 100 higher in latest Omicron-driven market swing
COVID-19: UK travellers visiting France will need negative coronavirus test as rules tightened over Omicron fears
Labour’s new shadow health secretary, Wes Streeting, said cancer cases will go undetected amid the backlog as he drew on his own experience with kidney cancer, which was only picked up because he was getting a scan for kidney stones.
Please use Chrome browser for a more accessible video player
The NAO said the “missing cases” will return to the NHS, although it cannot be certain how many, and the NHS will “need to increase its activity to meet this surge in demand”.
“Even if it can adapt, the scale of the challenge it faces is daunting,” the report says.
“If 50% of ‘missing’ referrals for elective care return to the NHS and its activity grows only in line with pre-pandemic plans, the elective care waiting list will reach 12 million by March 2025.
“If 50% of ‘missing’ referrals return and the NHS can increase activity by 10% more than was planned, the waiting list in March 2025 will still be 7m.”
Saffron Cordery, deputy chief executive of NHS Providers, which represents NHS trusts, told Sky News dealing with the backlog is “immensely challenging”.
She said the NHS is under “immense pressure”, with the new variant, the backlog, “huge staff vacancies” and “huge pressure on urgent and emergency care and other services, including mental health and community services”.
“I think it’s fair to say that the NHS is kind of on stand-by to expand its capacity, should it need to do that,” she added.
“It does come at a cost that… will be potentially cancelling routine operations, longer waits for people who come in to A&E, for example, so we know that those challenges are there.”
The NAO’s assessment found pre-pandemic the NHS was doing more work each year but demand for services was increasing even faster and there was an inequality in types of staff that increased.
Follow the Daily podcast on Apple Podcasts, Google Podcasts, Spotify, Spreaker
Between 2010 and 2019, the number of consultants grew at more than 3% but there was almost no change in nurse numbers while there was an annual 1.1% reduction in the number of general and non-critical care beds available for overnight use.
The report said there were several issues that needed to be tackled to address the upcoming surge in demand for elective care.
They include extra beds and operating theatre capacity beyond pre-pandemic planned levels, managing staff pressures, including long-standing staff shortages, and ensuring existing health inequalities are “not perpetuated or exacerbated”.